One Abutment One Time (OAOT) is a surgical protocol where a definitive prosthetic component is installed immediately upon implant placement. This approach was first described by Dr. Luigi Canullo in 2010. When it is time for the final restoration, the impression—whether analog or digital—is taken at the abutment level rather than the traditional implant level. Technically, this transforms a bone-level implant into a tissue-level implant (similar to the Straumann Standard Plus), but with the added advantage of tailoring the gingival height to the optimal level for every specific indication.
Advantages of the OAOT Approach
- Surgical Efficiency: It eliminates the need for a second surgery since the soft tissue heals around the already-exposed prosthetic component. While a healing abutment achieves this in an implant-level approach, the OAOT protocol streamlines the transition to the final restoration by using the definitive component from the start.
- Immediate Position Verification: It allows the clinician to correct the implant position by making the future gingival margin clearly visible. If the implant is too shallow, it can be submerged further to ensure a favorable emergence profile. Conversely, if the 3D position is compromised (too buccal or lingual), it is better to reposition it immediately rather than struggling with a difficult restorative path later.
- Protection of Peri-implant Tissues: This is the most critical yet debated point. Logic dictates that by connecting components further away from the bone and connective tissue fibers, we reduce the risk of introducing infection into the sensitive micro-gap where bone, implant, and soft tissue meet. While authors and clinical studies offer varying support, the biological imperative to prevent recession by minimizing trauma remains a primary driver.
- Structural Support: The protocol provides immediate support for soft tissue, which in some cases can reduce the necessity for bone or soft tissue augmentation.
- Controlled Emergence Profile: It facilitates the creation of a concave contour apically that transitions to a convex contour coronally, which is ideal for long-term stability and aesthetics.
Contraindications and Disadvantages
- Healing Requirements: OAOT is contraindicated when an implant must be submerged for protected healing, such as in cases involving simultaneous lateral window sinus lifts or extremely soft bone.
- Component Selection: There is a risk of selecting the wrong gingival height at the time of surgery, though this can be corrected.
- Clinical Demand: It requires the surgeon to determine the prosthetic level immediately and demands high primary stability, ensuring the implant torque exceeds the torque required for the final abutment connection.
The histology of Peri-implant complex
The place where the bone, soft tissue and crestal part of titanium implant meet is a very sensitive area where many structures depend on each other.
In modern implant design, maintaining the integrity of the “Mucointegration” is paramount. Every time a healing abutment is removed to take an impression or try in a framework, this delicate biological seal is torn, forcing the body to re-establish the attachment at a more apical level.
Dr. Giacomo Fabbri has highlighted the concept of the ‘Biological Room’; while implants lack the Sharpey’s fibers found in natural teeth, the similarities in soft tissue protection are striking. Implants rely on a Junctional Epithelium that connects to the titanium surface via delicate hemidesmosomes. The repeated connection and disconnection of healing abutments, impression transfers, temporary components and then final abutments, disturb these attachments, triggering an inflammatory response that forces the apical re-establishment of the biological width.
The Evidence Gap: Data vs. Reasoning
Numerous clinical studies have attempted to validate or dispute this protocol, primarily using marginal bone loss as the metric. Results are mixed: many show no significant difference between OAOT and repeated disconnection, while others demonstrate superior bone preservation over time.
The inherent difficulty in clinical dentistry is the “noise” within empirical data; countless patient variables—from systemic health to local biomechanics—are nearly impossible to isolate in a single study. When clinical results appear contradictory, we must distinguish between this statistical noise and the “purity” of biological logic. Furthermore, establishing definitive scientific proof is complicated by methodological bias; a significant challenge is that few studies are performed by truly neutral clinicians. Instead, they are often conducted by practitioners who already show a clear preference for either the OAOT or the traditional protocol from the outset.
However, scientific evidence is a mosaic, not a single data point. When empirical studies are inconsistent, we must look to mechanistic reasoning—in this case, the biological imperative to protect the mucosal seal by minimizing trauma. Reasoning based on known physiological principles can be just as compelling as a conflicted meta-analysis. By analyzing the biomechanical and histological advantages of OAOT, we find a logical “proof” that transcends the limitations of current trials.
Conclusion
If we adhere to the principles of Graft-Free Implantology, we must account for all aspects of the OAOT protocol. Even in scenarios where bone preservation might appear equivalent, the aesthetic and functional predictability—combined with a clear socioeconomic advantage—makes this protocol a superior choice for the modern clinician.
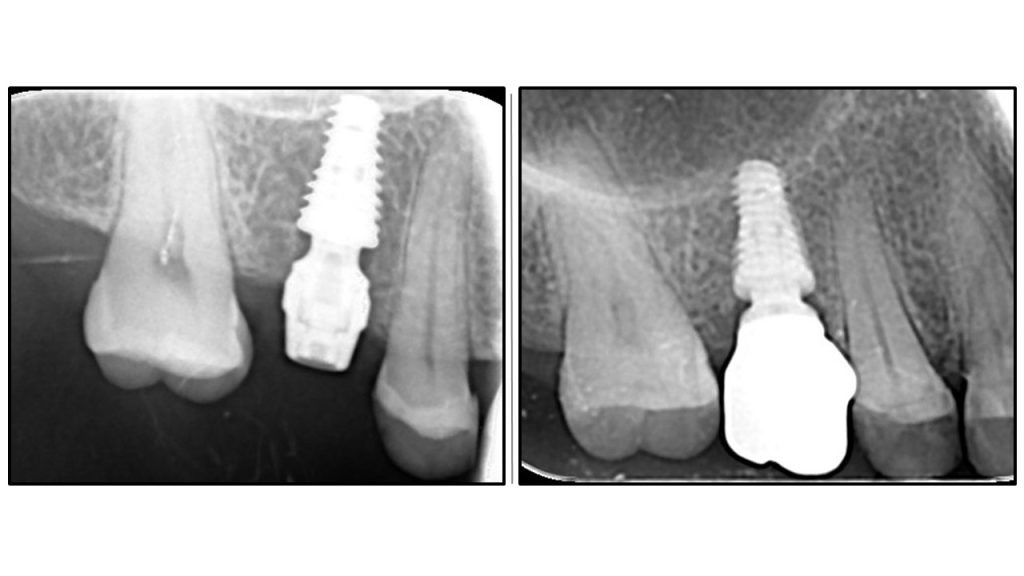
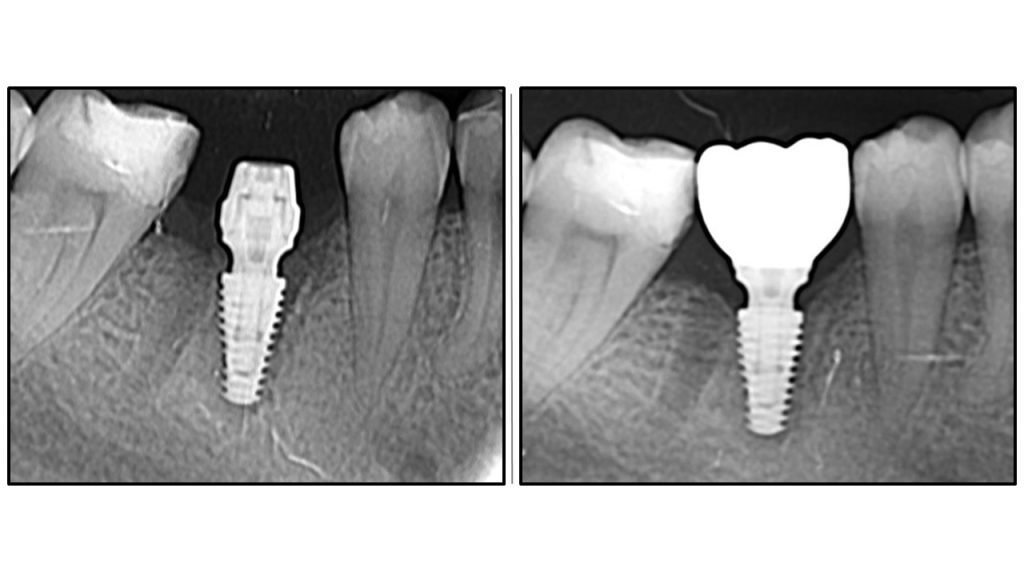
Radiographic Analysis: Crestal Bone Stability
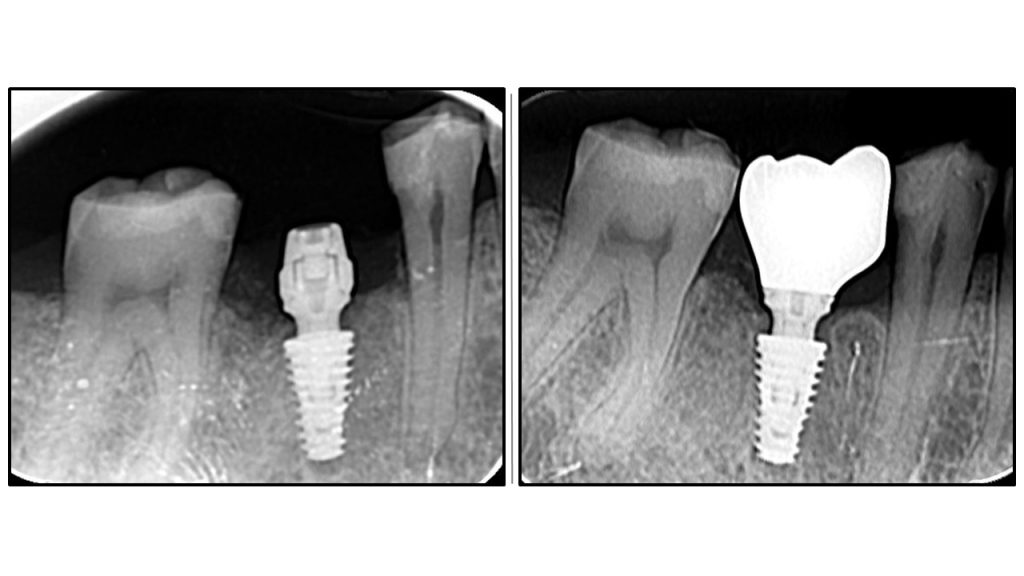
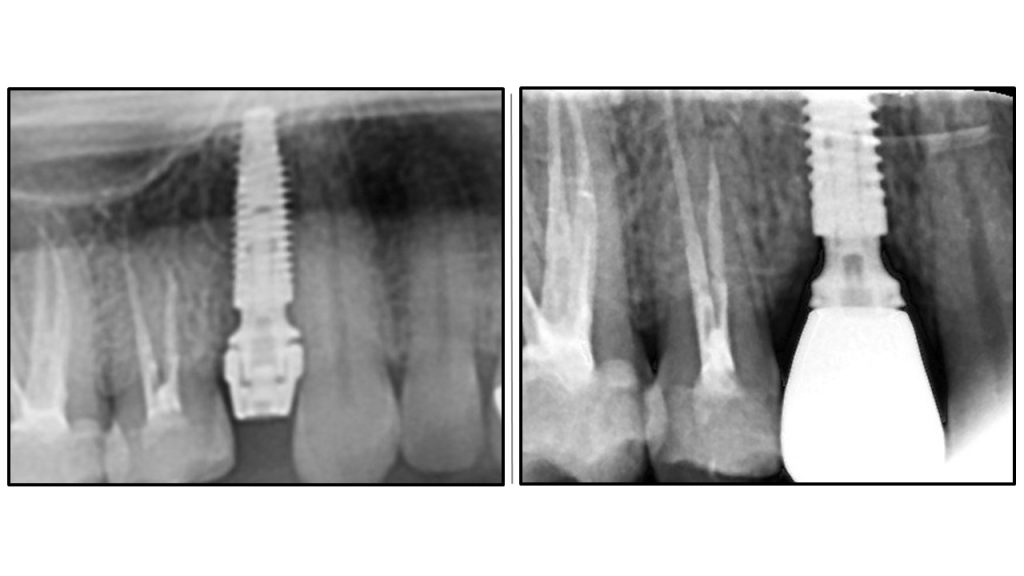
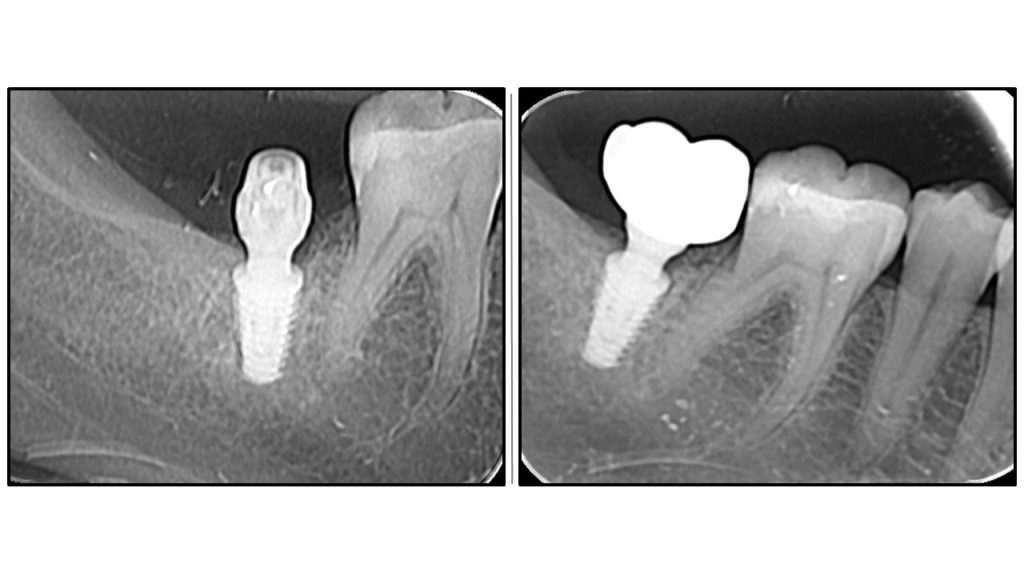
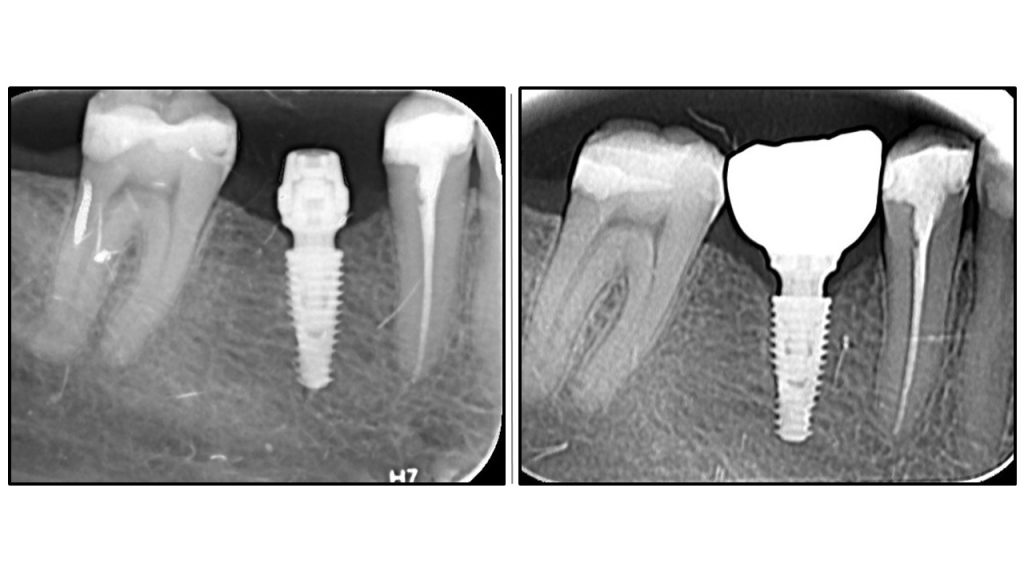


Leave a Reply