Is implant success rate known
Implant success rate is a very important topic and we mostly use it to reassure our patients that dental implant therapy is safe and successful, but it is also used internally to evaluate the treatment success. Or at least it should be. In Graft Free Implantology concept it is definitely important.
But in simple conversations, with patients, we usually tell them that the implant success rate is 98% and then we explain that it means that of every 50 implants we place, we lose one. Ok, that’s not so bad. Not gonna happen to me, the patient says.
But where did we get that number 98? There are many studies that flaunt with those numbers and there are some studies that show slightly lower success rates of 97, even 95% But we like the 98% number. Why? Well, it is pretty high number, everybody knows that 100 is impossible, and 99 sounds a bit fake, a bit too optimistic, but 98 sounds realistic. So, we keep it and use it.
But what does failure mean? It means we lose an implant. We place the implant, the implant doesn’t osseointegrate and falls out or we have to remove it. But what about implants that are stable, osseointegrated, but their position is not optimal and we have aesthetic failure? That surely can’t be successful implant, right?
So, the 98 number we tell everyone is really the Implant survival rate, not the success rate. Success should be measured by all the metrics: Aesthetics, function and reliability (reliability meaning there are no complications, no infections and no significant bone loss over years). And we should include time in our success rate. It must be defined as “ over 5 years”, “over 10 years” etc.
Also, it is not the same if we are restoring one tooth, with one implant, or a toothless segment with two implants ot a full arch. The survival rates are different and so is the success rate.
So, now we are realizing that Implant success rate might be slightly lower than 98 we talk about so confidently.
In fact, there are studies that show very different survival rates depending on the number of implants, by many clinicans. Most notable being Dr. Bjarni Pjetursson and his work:
For single implant restorations, he reports 5-Year Survival: 96.8% for implants) and 94.5% for crowns and for 10-Year Survival: Drops to approximately 89.4% for the restoration (1).
Dental bridges are a bit lower with 5-Year Survival: 95% for the bridge and 10-Year Survival: Drops significantly to 86.7% (2).
Dieter Busenlechner showed, in his study (8.) that the implant success rate ranges from 95.8% to 97.9% with a mean 97% success rate. Maybe from that 97.9% success rate we get the 98 number.
And those studies don’t even deal with other metrics we talked about, the aesthetics, function and reliability. It becomes clear that there is no One true number for implant success rate.
To provide a real-world perspective, I recently audited my own clinical outcomes. In fact, my records show that I have placed 2400 implants in the last 4 years and lost 80 implants. That would be a little less than 97% survival rate. But keep in mind, that is for all implants combined, from single tooth cases to full arch reconstructions.
While this 96.7% survival rate across thousands of implants provides a solid clinical benchmark, it remains a retrospective snapshot of a single practitioner’s experience. To truly move from observation to prediction—to understand the real risk our patients face—we must move beyond anecdotal data.
The theory of probable success rate
As dentists, we frequently claim to follow evidence-based practices, yet we often overlook the most fundamental of all scientific methods: mathematics. We treat retrospective clinical data as the beginning and end of ‘evidence,’ forgetting that Probability Theory is what actually allows us to translate those past results into future risks.
To simplify, we can define an implant failure as an unwanted event — a standard term in probability theory. If we treat 50 patients with single implants, assuming an optimistic 98% survival rate, each case represents an independent event. To calculate the cumulative risk of encountering at least one failure across this group, we apply the rules of probability for independent events, specifically the Addition Rule for Probabilities.
In simple terms, if you place an implant in Patient A (PA) and another in Patient B (PB), the probability that at least one of them will experience a failure is not a simple 2%. It is not 4% either. Why do we subtract the product (PAXPB)? In mathematics, this product represents the “overlap”—the rare scenario where both implants fail simultaneously. If we don’t subtract it, we are effectively double-counting that specific failure. Mathematically, it is expressed as:
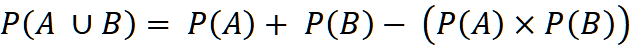
If we plug in our “optimistic” 2% failure rate:
0.02 + 0.02 – (0.02 × 0.02) = 0.0396
This translates to a 3.96% failure rate the moment you have just two implants “in the wild.” While we like to think of each surgery as a fresh start, the mathematics of a dental practice is cumulative. By the time you have placed 50 implants, the probability that you will have at least one “unwanted event” isn’t a matter of bad luck — it is a statistical certainty.
Using the Complement Rule, the probability of having a “perfect” record with 50 implants is (0.98)50 is only about 36%. This means there is a 64% chance that at least one implant will fail.
The Surgeon’s Paradox: As you become more successful and place more implants, your individual success rate might stay at 98%, but your mathematical ‘certainty’ of facing a complication increases every single day. The better you get, the more failures you will technically manage. Math proves that the master surgeon isn’t the one who never fails—it’s the one who is best prepared for the inevitable 63.6%.
When we tell a patient “98%,” we are describing a single event in a vacuum. But as clinicians, we don’t live in a vacuum; we live in the cumulative reality of our total caseload. This realization is the first step in understanding why we must look for concepts that reduce the number of variables—and thus the number of opportunities for failure.
Now, let’s address the survival rate of a full arch case. Many doctors prefer FP1 cases on 6 implants and consider that approach a gold standard. Because the gums are visible, implants need to be in precise positions of the teeth they restore. So, if one implant fails, the whole case fails, because, once you lose that implant, bone resorption will follow, gums will recede and it will be no easy feat to restore that.
The probability of this “system failure” is calculated using the Multiplication Rule for independent events (Pn). If we assume a standard 98% survival rate for each individual fixture, the math for a 6-implant system looks like this:
0.986 ≈ 0.885
This means the “Gold Standard” FP1 approach actually carries an 11.5% risk of system failure. We are essentially asking our patients to accept a 1-in-10 chance that their entire complex, expensive reconstruction will fail because of a single point of weakness.
But the math gets even more unforgiving when we realize that these are not isolated events. To achieve that “Gold Standard” FP1 aesthetic, we almost always rely on Guided Bone Regeneration (GBR).
This introduces Dependent Events. The survival of the implant is now tethered to the success of the graft. If we take a conservative complication rate for GBR of 10% (90% success), we have to multiply that risk across every site.
Mathematically, the probability of a “perfect” 6-implant FP1 case requiring grafting is:
(PGraft X PImplant)6
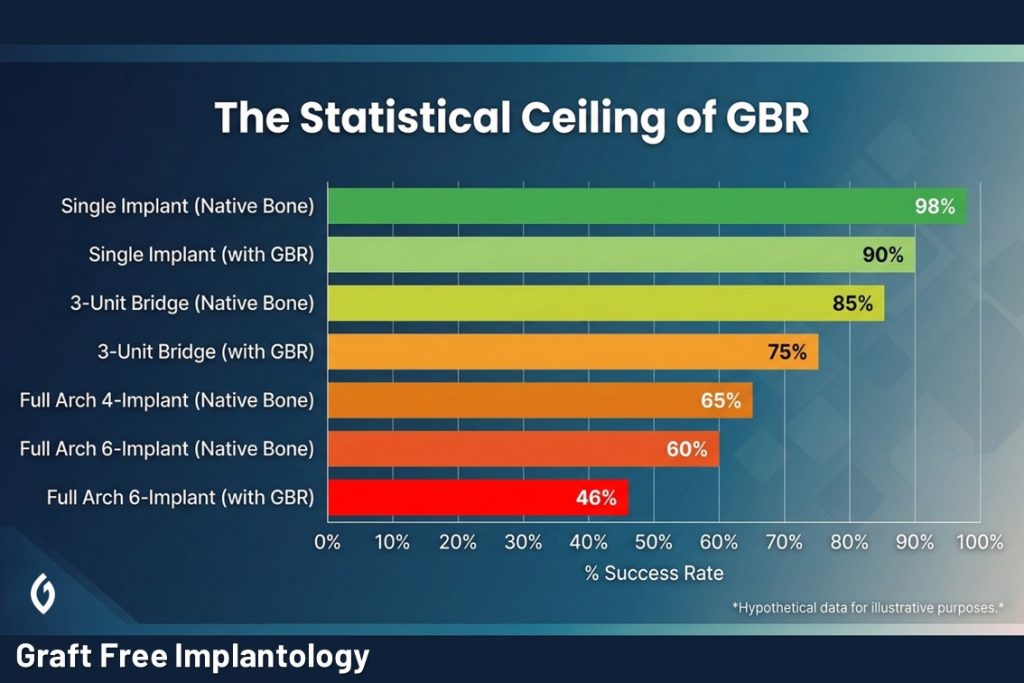
(0.90 X 0.98)6 ≈ 0.46
This result is startling. We are essentially proposing a treatment plan where there is a less than 50% chance that the entire reconstruction will remain complication-free over the long term. This isn’t because the surgeon is unskilled or the implants are poor; it is because the system architecture itself is mathematically fragile. By tethering success to a chain of twelve events—where six independent sites each rely on the conditional success of a graft and an implant—we have created a ‘statistical ceiling’ that makes long-term perfection nearly impossible to achieve.
In probability, this is often called a Serial Reliability Model. In such a system, the strength of the whole is dictated by its weakest point; if any one of those twelve links in the chain breaks, the entire case is compromised.
Is there evidence to mathematical hypothesis?
What about real world results? The real data that the clinicians are reporting?
Well that is a bit difficult to interpret, because there are many different techniques and materials. Also, the metrics of success is not the same.
The Milan group, led by Dr. Filippo Fontana (3.), analyzed literature and reported various complication rate ranging up to 50%. They also classified GBR complications into 4 classes:
- Class I – exposure less than 3mm without purulent exudate
- Class II – large device exposure (>3 mm) without purulent exudation
- Here, the author suggests removing the non-resorbable membrane and salvaging the graft.
- class III: device exposure with purulent exudation
- Basically treated similar to class II, but with some graft manipulation in order to save it.
- class IV (a and b): abscess formation without device exposure
- Class IVa – Here, the abscess is located under the membrane and the treatment requires complete removal of the grafting material. Basically, this is total failure.
- Class IVb – The exudate is found over the device and this should have better prognosis, but still the non-resorbable membrane should be removed, graft saved and resorbable membrane placed.
Their conclusion is “Although the GBR technique is considered to be a predictable surgical procedure, further modifications in materials and techniques are being developed in order to reduce clinical complications. Adherence to proven clinical protocols and the introduction of new materials could reduce the incidence of complications and increase the predictability of bone augmentation.”
In the world of engineering and mathematics, this is known as Optimizing a Fragile System. Instead of changing the system to make it robust, they are trying to make a fragile process “work” through sheer precision.
And this is a reoccurring theme in GBR reports. Whenever a complication occurs, or the rate is higher then the author would like to, they wish for better materials.
“However, there are still challenging situations and complications which necessitate future developments of GBR membranes.” Is a conclusion by dr. Ibrahim Elgali in his review “Guided bone regeneration: materials and biological mechanisms revisited” (5.)
Zeinab Rezaei Esfahrood and associates, in their review of the literature of Short dental implants in the posterior maxilla,found that “implants placed in pristine bone had a higher survival rate (96.4%) compared with those placed in an augmented sinus (86.1%)”. (6.)
As Dr. Lim et al. concluded in their 2018 meta-analysis (4.), the 16.8% complication rate in GBR is independent of the ‘latest and greatest’ membranes. Instead, it is tied to technique sensitivity. For us as clinicians, this means that even with the best materials, we are operating within a system that has a built-in high failure rate due to its extreme sensitivity to soft tissue variables. We are not just fighting biology; we are fighting the mathematical law of diminishing returns that governs technique-sensitive, multi-step procedures.
Even Urban et al. (2019) reported a 17% complication rate specifically for vertical augmentation using reinforced dPTFE membranes.
Let’s address another study by Duong T. Tran “Survival of Dental Implants Placed in Grafted and Nongrafted Bone: A Retrospective Study in a University Setting” (9.) They report this “A total of 1,222 patients with 2,729 implants were included. The cumulative survival rates at 5 and 10 years were 92% and 87% for implants placed in native bone and 90% and 79% for implants placed in grafted bone, respectively.” but they conclude this “There was no difference in the dental implant survival rate when implants were placed in native bone or bone-grafted sites. Smoking and lack of professional maintenance were significantly related to increased implant loss.” How can their conclusion differ from the results they are reporting? Am I misinterpreting?
The discrepancy lies in the difference between Clinical Significance (the absolute numbers) and Statistical Significance (the P-value). When the authors say there was “no significant difference,” they are referring to the Multivariate Analysis (Cox regression). Mathematically, because the study was retrospective and the sample size of 10-year follow-ups might have been smaller or more “noisy” (with variables like smoking and maintenance taking up more “weight” in the calculation), the P-value didn’t cross the magic threshold (usually P < 0.05). In researcher-speak: “The difference exists (87% vs 79%), but we can’t prove it wasn’t due to random chance or other factors like tobacco.” In reality, 87% vs. 79% is an 8% absolute difference in survival at 10 years.
Sanz-Sanchez also discussed the complication rate of bone grafting procedures and offered their classification. They, too, found the range of 0 to 45% complication rate with a mean of 16.8% but concluded differently than others that “It is therefore recommended that whenever possible clinicians choose procedures that have a lower degree of complications and employ less invasive surgical interventions.”
There are almost no clinical studies, papers that deal with late bone grafting complications, but they exist. It is not seldom found that the graft was compromised during healing, somehow the complications were dealt with, healing concluded, but years later found that the grafted bone isn’t that solid, that there were zones in the middle with bone substitute present and if we were to drill into it, we would find sand.
Arne Mordenfeld found that “DPBB particles were found to be well integrated in lamellar bone, after sinus floor augmentation in humans, showing no significant changes in particle size after 11 years.” (7.) And while many proponents of GBR find this result as a success and testament to grafting, from biological point of view it might be viewed as failure. This is no human bone anymore. Vital bone can remodel, heal, and fight infection. A bovine bone particle cannot. It is a “stone in a wall.” If the “mortar” (the 50% vital bone) is ever compromised by peri-implantitis, the “stones” (the particles) have no defence mechanism.
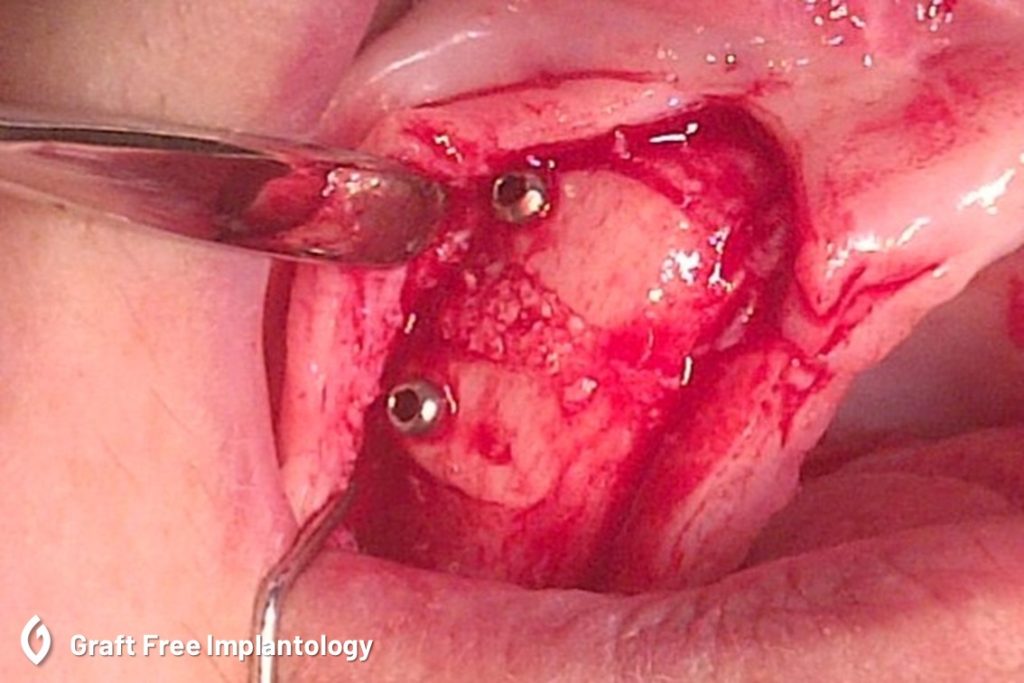
You could argue that all those complication rates are not failure rate. In fact, Istvan Urban reports 17% complication but only 3% total failure. But there lies the problem. Let’s consider that most reported complications of GBR are flap dehiscence and membrane exposure. First of all, why did this happen in the first place? Too much flap tension? I don’t think so. Most often reason for flap dehiscence is poor vascularization. That whole area, the graft, the bone and soft tissues, need blood supply and since there is a foreign body, a membrane which is either semipermeable or not at all, and the bone substitute material below it, is making vascularization more difficult. Especially if the over correction principle is involved. In fact, the dr. Urban acknowledges the problem of vascularization in his article saying that “regenerating area con-fined by the membrane might rely solely on nourishment from the basal bone vasculature.” (10.)
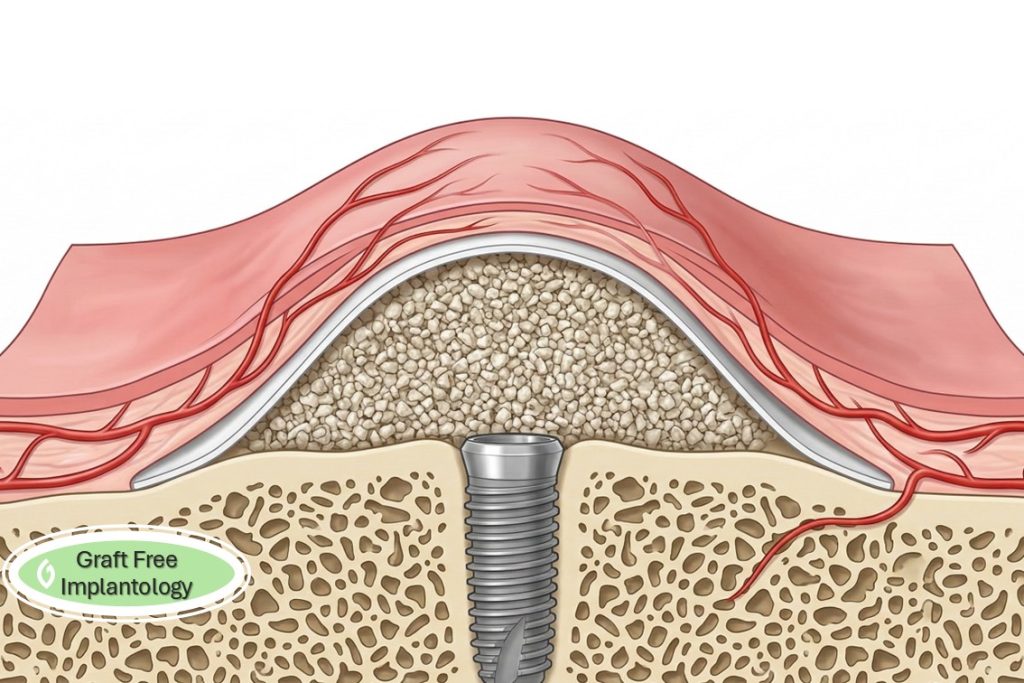
So, now you deal with the complication, you rinse everything, you give more antibiotics, the dehiscence finally closes, the site heals and you call it a win. But what is happening to the graft below is a great unknown. Since there was a dehiscence, the final result should be in question. Dr. Sanz-Sanchez says “The complications associated with these interventions (GBR) are usually related to exposure of the barrier membrane, which may impair the outcome of the regenerative procedure, because the exposed membrane immediately becomes contaminated with bacteria from the oral environment.”(11.)
Discussion
Bias
First of all, let’s deal with the fact that there is so many different results and conclusions. Why? Well, we have to account that we are all human beings and very susceptible to Bias.
In science, bias is any systematic error that results in an incorrect estimate of the association between exposure and outcome.
1. Confirmation Bias (The Most Common)
This is the tendency to search for, interpret, and recall information in a way that confirms one’s pre-existing beliefs.
- In Implantology: A surgeon who believes GBR is “predictable” will focus on the 83% success rate in a study but ignore the 17% complication rate as “outliers” or “bad luck.”
- The Trap: They see what they want to see on the X-ray (solid white) and ignore what they don’t (lack of vital bone).
2. Expectancy Bias (The “Observer-Expectancy” Effect)
This happens when a researcher’s cognitive bias causes them to subconsciously influence the participants or the data to reach a desired result.
- The “Wish”: This is exactly what we find in the studies. The authors expect GBR to work, so when it doesn’t, they conclude that “better materials” or “better technique” will fix it, rather than questioning the method itself.
3. Publication Bias (The “File Drawer” Problem)
Journals are much more likely to publish “positive” results (e.g., “Grafting worked!”) than “negative” results (e.g., “Grafting failed to produce bone”).
- The Illusion: This creates a skewed body of evidence. Clinicians think GBR is more successful than it is because the failures often remain unpublished in the “file drawer.”
4. Selection Bias
This occurs when the “success” data comes from a highly filtered group (e.g., non-smokers with perfect hygiene and massive amounts of existing bone).
- The Reality: When these methods are applied to the “real world” of a general practice, the PSuccess drops significantly, but the “Gold Standard” label remains.
5. Sunk Cost Fallacy (Cognitive Bias)
While not a formal “research bias,” this is huge in clinical circles. If a dentist has invested time and money in GBR training and materials, they are psychologically resistant to the idea that grafting is risky.
Other reasons
Other than bias, there could be other reasons for adherence to GBR being the Gold standard:
1. The Industrial-Academic Complex
This is perhaps the most “unspeakable” reason in formal literature.
- The Revenue Model: GBR is a massive economy. Between membranes, bone substitute materials, fixation screws, and specialized kits, a single GBR case generates significant revenue for manufacturers.
- The Funding Loop: Much of the high-level research (RCTs) is funded by the very companies that produce these materials. It is rare to see a large-scale study funded to prove that not using a product (the GFI approach) is superior.
2. The “Recipe” vs. “Surgical Art”
GBR has been successfully marketed as a standardized protocol.
- Teachability: It is easier to teach a “recipe” (Place Bone -> Place Membrane -> Close) in a weekend course than it is to teach the deep biological understanding of sub-crestal dynamics or advanced site preparation that GFI often requires.
- The Safety Net Illusion: Surgeons often feel that by “adding” material, they are actively fixing a problem. Doing “less” (GFI) can feel counterintuitive or even “risky” to a clinician trained in a additive mindset.
3. Definition of “Success” in Literature
As noted with the Istvan Urban example, the “Gold Standard” stays gold because we define success too narrowly.
- If the implant is stable and the patient isn’t in pain, it’s a “success,” even if the “bone” around it is actually just encapsulated xenograft.
- Cognitive Dissonance: Admitting that a 17% complication rate is a failure of the philosophy would require a generation of surgeons to admit they have been over-treating or mis-treating patients for decades.
Conclusion: From Statistical Survival to Biological Success
We must change our mindset. Survival rates are not success rates. A “surviving” implant can still be a biological or restorative failure. To move forward, we must define a successful outcome as an amalgamation of six core metrics that must remain stable over time:
The Six Pillars of Success
- Function: The restoration must be functional, with correct occlusion and a design that allows for self-cleaning, preventing food impaction and infection.
- Reliability: Long-term stability of the peri-implant tissues and a lack of prosthetic complications.
- Safety: Minimizing intraoperative complications and avoiding damage to anatomical structures—adhering to “primum non nocere.”
- Simplicity: A streamlined surgical workflow that allows for a predictable, successful outcome every time.
- Aesthetics: The final result must satisfy both the patient and the practitioner. What is visible must be beautiful.
- Socio-economic Aspect: We must respect the patient’s investment of both time and money.
These metrics are not a hierarchy; they are equally vital. This is the Graft Free Implantology (GFI) way.
The Paradox of Failure
It is better to lose an implant early than to allow a poorly positioned implant to osseointegrate. While this is a difficult concept for many clinicians to accept, we must realize that an early failed implant is a manageable complication during the treatment phase, not a failure of the case itself. If we are dedicated to fulfilling all six metrics, the statistical reality changes in our favor.
The GBR Reality Check
We need more scrutiny and objectivity regarding Guided Bone Regeneration. We must account for the 17% complication rates and what they truly signify for the patient’s biological future.
Why, for example, would we plan an FP1 full-arch restoration for a patient with a high smile line, requiring massive regeneration just to achieve an even gingival line, when there is a “ticking bomb” of potential late-stage complications woven into that very treatment?
Final Thought
The core philosophy of implant dentistry needs to evolve. Part of that evolution involves redefining what a failed implant actually signifies. If an implant is lost but can be replaced without compromising the final prosthetic result, we should not view it as a clinical catastrophe, but as a bump in the road. However, this perspective requires a fundamental shift in how we work: we must stop planning for a ‘perfect’ scenario and start planning for resilience. We need to design treatment plans that account for possible biological setbacks, ensuring that our final goal remains reachable even when the path isn’t linear.
Ultimately, we must ensure success for every patient in our daily practice—not just for the select, pristine cases that find their way into glossy journals. By prioritizing biology over foreign materials and planning for contingencies, we choose a path of predictability, longevity, and true clinical excellence.
Comparison of Clinical Priorities
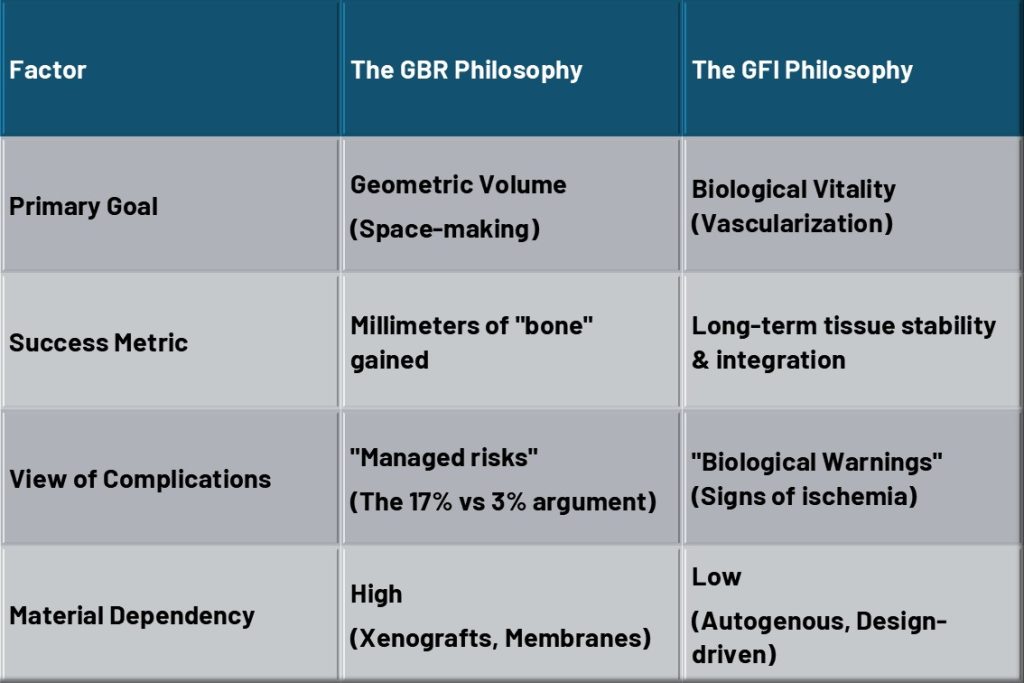
Literature
- Jung, Pjetursson, et al. (2008 & updated 2012).
- Pjetursson et al. (2012) – Systematic Review of FDPs.
- Fontana, F., Rocchietta, I., & Simion, M. (2011). Complications in guided bone regeneration. The International Journal of Periodontics & Restorative Dentistry, 31(3), 263–271.
- Lim, G., Lin, G. H., Monje, A., Chan, H. L., & Wang, H. L. (2018). Wound Healing Complications Following Guided Bone Regeneration for Ridge Augmentation: A Systematic Review and Meta-Analysis. The International Journal of Oral & Maxillofacial Implants, 33(1), 41–50.
- Elgali I, Omar O, Dahlin C, Thomsen P. Guided bone regeneration: materials and biological mechanisms revisited. Eur J Oral Sci. 2017;125(5):315-337. doi:10.1111/eos.12364
- Esfahrood ZR, Ahmadi L, Karami E, Asghari S. Short dental implants in the posterior maxilla: a review of the literature. J Korean Assoc Oral Maxillofac Surg. 2017;43(2):70-76. doi:10.5125/jkaoms.2017.43.2.70
- Mordenfeld A, Hallman M, Johansson CB, Albrektsson T. Histological and histomorphometrical analyses of biopsies harvested 11 years after maxillary sinus floor augmentation with deproteinized bovine and autogenous bone. Clin Oral Implants Res. 2010;21(9):961-970. doi:10.1111/j.1600-0501.2010.01939.x
- Busenlechner D, Fürhauser R, Haas R, Watzek G, Mailath G, Pommer B. Long-term implant success at the Academy for Oral Implantology: 8-year follow-up and risk factor analysis. J Periodontal Implant Sci. 2014;44(3):102-108. doi:10.5051/jpis.2014.44.3.102
- Tran DT, Gay IC, Diaz-Rodriguez J, Parthasarathy K, Weltman R, Friedman L. Survival of Dental Implants Placed in Grafted and Nongrafted Bone: A Retrospective Study in a University Setting. Int J Oral Maxillofac Implants. 2016;31(2):310-317. doi:10.11607/jomi.4681
- Urban, I.A., Serroni, M., Dias, D.R., Baráth, Z., Forster, A., Araújo, T.G., Saleh, M.H.A., Cucchi, A. and Ravidà, A. (2025), Impact of Collagen Membrane in Vertical Ridge Augmentation Using Ti-Reinforced PTFE Mesh: A Randomised Controlled Trial. J Clin Periodontol, 52: 575-588. https://doi.org/10.1111/jcpe.14129
- Sanz-Sánchez I, Sanz-Martín I, Ortiz-Vigón A, Molina A, Sanz M. Complications in bone-grafting procedures: Classification and management. Periodontol 2000. 2022; 88: 86–102. doi:10.1111/prd.12413

Leave a Reply